The Celebration of a Miracle
One-year-old and family return to the ICU to thank the medical team that saved his life
It was all smiles on the fourth floor as pediatric intensive care nurses at St Vincent Healthcare greeted Caleb Hyland and his mother, Lindsey, in early December. The doctor and four nurses who welcomed them remembered Caleb and his family well. Almost a year earlier, he had spent two weeks under the care of the team, and there were times when they weren’t sure he’d make it.
But on this day, there was nothing but joy over the fact that the baby had made a complete recovery. In celebration of his first birthday, it was important to Lindsey to come back to the people that had cared for her son and celebrate his miraculous recovery.
“Oh my gosh, he’s gotten so big! And look at that smile,” one nurse said.
“He’s so healthy!” another added.
Late last year, when Caleb was just 7 weeks old, he came down with RSV — respiratory syncytial virus. Though it’s highly contagious, most children have built up their immunities to it and endure sniffles or cold-like symptoms. For some babies it is far more serious and at times a deadly threat.
“Infants under 2 months are especially susceptible because their immune system is not yet developed and their lungs are so tiny,” says Dr. Menard Barruga, physician of pediatric critical care medicine, and Caleb’s doctor. “There’s no way to completely prevent it, especially if there are older children in the home or if the baby has been exposed.”
Only 5 percent of those who contract RSV will need hospitalization but, as Barruga says, “It happens and it’s very scary for parents.”
The Christmas holiday was busy at the Hyland house. In addition to Lindsey and Chaz and their little boys, Caleb, and 18-month-old Zach, Chaz’s older children, London, 11, and Sayre, 10, were visiting.
The day after Christmas, Lindsey says Caleb slept most of the day. He woke up twice to eat instead of the eight times he normally nursed during the day. She attributed it to being overstimulated and tired.
“When we bathed him that night, he was very lethargic, but he wasn’t feverish, and his breathing wasn’t labored. But when I went to change him later his ribs were protruding. It terrified me. I told Chaz I was taking him in.”
The nurses at the Red Lodge hospital were certain it was RSV and that he was in serious condition. Lindsey and Caleb were rushed by ambulance to Billings.
“In the 10 minutes since I’d left home, his lips were turning blue, and I could see the veins in his face,” Lindsey says with tears in her eyes.
At St. Vincent Healthcare, the nurses reflected on last year’s RSV season. Amanda Whiters, PICU nurse, says the number of RSV patients in PICU that they handled last year was high the entire RSV season, which usually runs from December until well after the first of the year.
“It started with a vengeance right after Thanksgiving and there was no respite,” she says. “It hit hard and lasted for several months after the new year.”
She, Christine Hebert and Kori Caudill are part of the team of registered nurses that are usually in one of the five pediatric ICU rooms at any given time. Lori Marosok, a floor nurse, usually cares for patients after they have progressed out of the PICU. All four nurses took care of Caleb at some point during his stay.
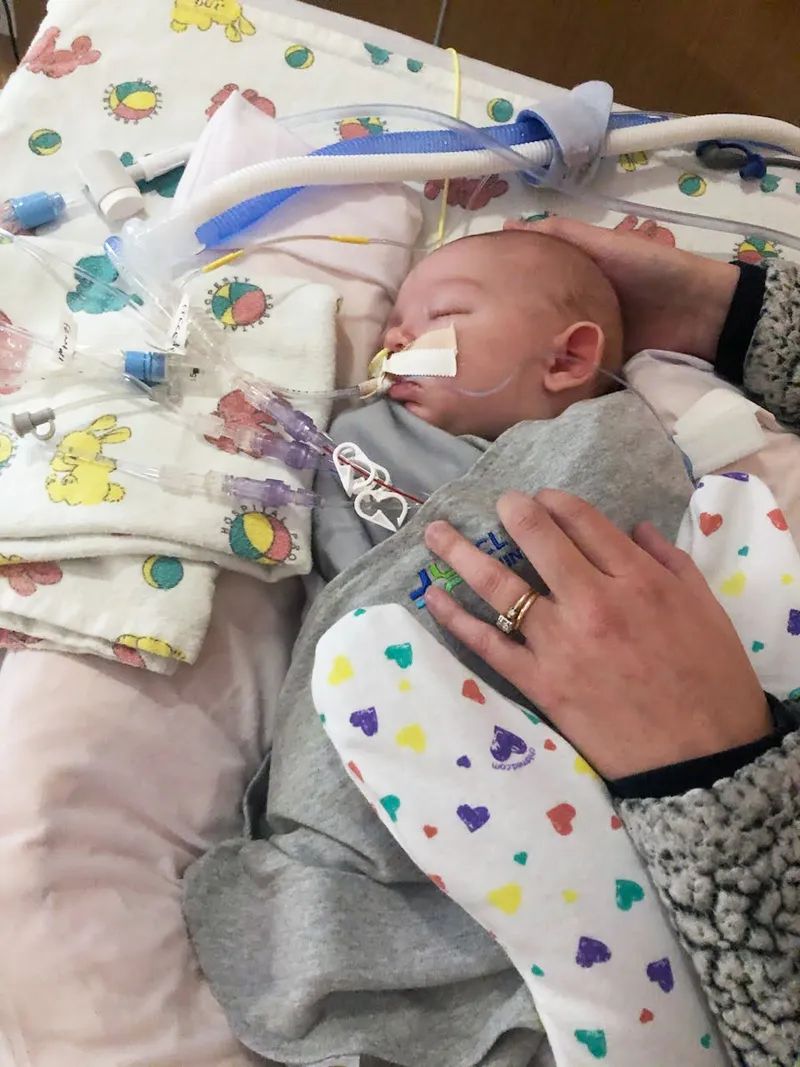
“He developed pneumonia along with RSV and immediately he was sedated with fentanyl and given a breathing and feeding tube,” Lindsey says.
“He was just too worn out to breathe on his own,” Barruga explains as he reflects back on Caleb’s situation. “He was weakened from his secretions and was a very sick little baby.”
RSV is known to run in cycles, usually every two years. Some believe that the pandemic played a role in the recent spike in severity. With children segregated from others, their immune systems weren’t prepared for the next RSV cycle and, as a result, cases rose rapidly.
On the PICU floor that cared for Caleb, there is a close-knit group of 28 nurses that have more than 263 combined years of experience dealing with very sick children. ICU Nurse Manager Mike LaBard has managed them for two years and has, himself, more than 24 years as a pediatric critical care and flight nurse.

“You don’t see what we have here in every hospital,” LaBard says. “I’m blown away by the dedication of these nurses. They put their all into their jobs. Hands down, this is the best and most compassionate ICU team I’ve ever worked with.”
“Someone was always with Caleb,” Lindsey remembers. “He was never left alone. They constantly checked his vitals and kept an eye on the monitors and they always told me what they were doing. As sick as he was, I knew he was in great hands.”
In the first week of Caleb’s time in the hospital, he showed very little progress and as a result remained sedated and hooked to life-support machines.
“We had people praying for him and he had the best of care possible, but nothing was happening,” Lindsey says. “I just wanted him to wake up so I could hold him in my arms. It was the most horrific thing I’ve endured as a mother.”
One week turned into two. Older brother Zach was being cared for by Lindsey’s parents, who live in Billings. When she could, Lindsey would rush over to see him and then hurry back to be near Caleb.
“That first week I wouldn’t leave his side,” Lindsey says. “But by the second week, the nurses convinced me that I needed to get rest, or I was going to get sick too.” She checked into the Ronald McDonald House across the street from the hospital and she and Chaz took turns staying with Caleb and being with Zach.
“It can be very stressful for parents,” Whiters says. “They’re scared, so we try our best to stay calm so that they do. We become like mama bears to them. We make sure they are eating, taking breaks and resting. It’s just what we do.”
After a week under sedation, Caleb finally turned a corner.
“He was weaned off the fentanyl slowly and after about four days of that, they were ready to take the breathing and feeding tubes out and see how he’d do,” Lindsey says.

Thankfully, the care given to him by the doctors and nurses, the power of prayer and Caleb’s fighting spirit prevailed, knocking out both the RSV and pneumonia.
“The first time I got to hold my baby after two weeks was the best feeling ever,” Lindsey says. “When he started nursing, I knew he’d be OK. He really is a fighter.”
At this time last year, LaBard says, the PICU was overflowing with RSV cases.
“We were at 150 percent of capacity. Our nurses did what needed to be done and did an amazing job caring for all the patients,” he says. “We want all of our patients to have the same outcome as Caleb did.”
“I’m so grateful that my baby is healthy,” Lindsey says. “It was a terrifying time, and I fully believe that Caleb would not be here if not for God’s mercy, the power of prayer and the care of the amazing doctors and nurses.”
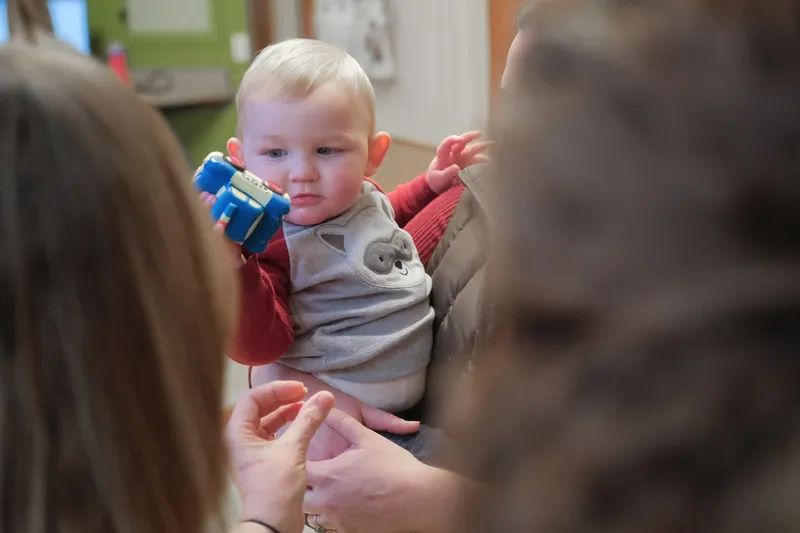
At the celebratory reunion, the nurses couldn’t help but fuss over Caleb, each taking a turn to hold the robust 1-year-old while visiting with Lindsey. It was clear this reunion was a special one for everybody.
“We don’t often get to see someone that’s been in our care after they leave,” says Marosok. “Having him come back to visit us this healthy and active is awesome. This is a special day for all of us.”
WHAT TO LOOK OUT FOR WITH RSV
The Signs & the Symptoms
In mild cases of RSV, you might see a runny nose, low-grade fever, sneezing and a dry cough. In more severe cases, you’ll find shallow, rapid breathing (tachypnea), retractions where the chest muscles and skin pull inward with each breath, a severe cough, lack of appetite, lethargy and irritability.