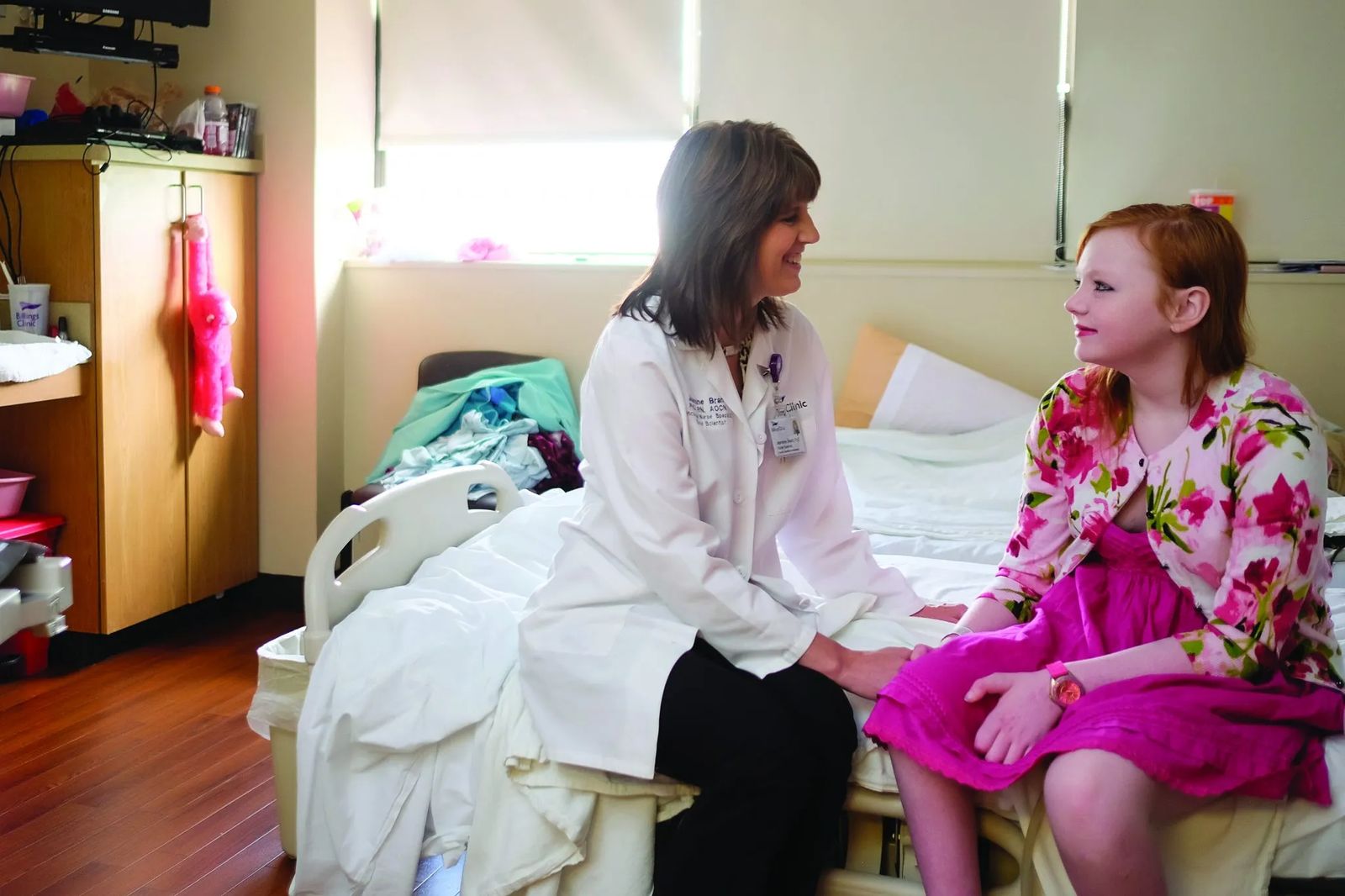
Cover Story: Jeannine Brant Touches the World
Hoping to change the face of cancer care
To listen to Jeannine Brant talk about her professional mission, you’d swear you were listening to a special operative talk about the threats on the job.
She travels a couple of times a year to the Middle East. She’s lucky. She only has to use one passport. Some of her colleges have to change passports in between their legs of travel so as not to leave a paper trail of their itinerary, she says as she explains the complexities of traveling between enemy countries. She’s registered with the State Department and gets alerts on her phone when there are terrorist threats nearby. During one trip, the plans completely changed when a threat emerged targeting the venue where she was a guest speaker. She’s never American when she travels. She pretends to be European instead, drawing on the little bit of Swedish she remembers from her days as a foreign exchange student. “We coordinate our stories before we go out,” she says about her journeys overseas.
Jeannine Brant doesn’t work for the Central Intelligence Agency. She’s not a diplomat. She doesn’t dabble in international trade. She’s a nurse scientist with the Billings Clinic who is trying her best to change the face of cancer care around the world. She’s an expert in palliative care and pain management and she’s trying to make sure that every patient, no matter what their color, background or religious preference gets compassionate care that can help them in their fight against cancer.
“I developed this passion for people in the Middle East. This project really caught fire in my soul,” Jeannine says today about her work with the Middle East Cancer Consortium. She never really thinks about the threats but instead loves looking into the eyes of the people she’s working with – the nurses and doctors delivering cancer care in these, often times, war torn countries. Imagine being a female nurse not being able to address a male doctor about a patient’s care. Think about the lack of drugs available to help someone in the midst of suffering. Consider the idea that you know a patient is terminal but you can’t share the news because it’s considered a cultural taboo. All of these things and more have a daily presence in cancer care in the Middle East.
“That's where my faith comes in. I put my total faith in the Lord. I know that things can happen and people think I'm crazy for going over there, but it's a passion. I see some amazing things happening because of the work that we’re doing over there and it's bigger than health care,” Jeannine says with emotion. “Health care is where it is starting, but it’s revolutionary in social change.”

Some might say Jeannine’s passion for palliative care was sparked by chance. Others might say it was fate when she marked her first day on the job as an oncology clinical nurse specialist in the summer of 1990 at St. Vincent Healthcare. After spending a few years getting her Masters in Oncology Nursing at the University of California, San Francisco, she was glad to be back home. As nurses often do, she checked the patient list, looking for familiar names. One name stuck out. Dave Ketterling was a high school friend she hadn’t seen in years. Her heart sank. “That’s the reality,” she says about her friend who hadn’t even hit his forties yet. “That’s tough. He was a young guy battling a sarcoma.”
When she walked into his hospital room, she hardly recognized the man lying in the bed. “He had been undergoing chemotherapy for a couple of cycles. He lost thirty pounds and couldn’t keep any weight on.” Nausea from the chemo was leaving him weak and without a whole lot of hope. “Back then, our philosophy was, ‘Let’s just put people to sleep with a lot of medication so that they don’t have to get sick.’ Despite those medications, he was still really sick.”
She immediately thought of her work at the University of California, testing a drug in a clinical trial that could prove to be a saving grace for her very ill friend. “One of the things that I had thought about was the fact that we were using this brand new medicine in San Francisco in a clinical trial called Ondansetron.” She asked the doctor overseeing Dave’s case if she could get approval to bring the drug to Billings. He agreed.
She had no idea what she was in for.
“It was a huge fight because they didn’t have it on the shelves yet,” Jeannine shares. The request went through an Institutional Review Board. Lawyers calculated the risks. She had to write a formal proposal. She called the pharmaceutical company direct to plead her case. It wasn’t easy.
“We finally did it. I was so excited. One of the things about being a young nurse is that you don’t see any boundaries,” she says with a smile. It’s a message she continues to share with nurses who work day in and day out at a patient’s bedside. “You can do it. If we stay focused on what is best for patients and their families, nothing is beyond reach. We can change the world.”
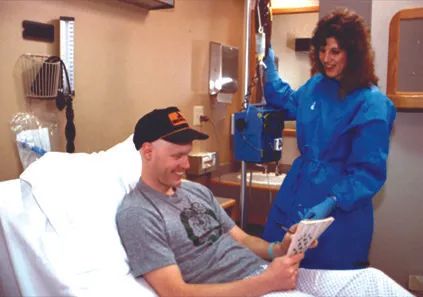
She won’t soon forget the day she personally administered this new drug to her dear friend. “I kept checking on him like a mother checks on her child. ‘How are you doing Dave?’ He finally said, ‘Hey, I am not feeling anything!’ Normally by that time he was throwing up. It was a miracle drug.” Within time, she says, “He gained his 30 pounds back while he was on chemotherapy. He started working again. He owned a small restaurant downtown.”
Little did Jeannine Brant know that this one act would help put her career on a new course.
First came an award-winning documentary journaling how this new medicine was drastically changing the quality of care and people’s lives. Jeannine and Dave were front and center in the film. Not long after, she was asked to speak at the Zofran launch, the marketed name for Ondansetron. Jeannine says simply, “It was really pivotal in my career.”
It wasn’t long after that Jeannine Brant got put on the map as a noted speaker and author for medical publications thanks to her passion and some, as she puts it, fabulous mentors. She laughs and says, “My first papers were probably horrible. But I kept doing it!” It was all sparked because she took a chance and fought for a patient in need. She smile and admits, “I’m kind of one that if I see something that needs to be done, I just do it. Sometimes I don’t think twice about it especially if it involves a patient’s wellbeing.”

When Jeannine Brant talks about her patients, it sounds as if she’s talking about family. She’ll laugh about the time she and a few fellow nurses popped some popcorn and took an entire floor of patients being treated for leukemia up to the hospital roof so that they wouldn’t miss the fireworks on the fourth of July. She talks about the recordings she helped one terminal patient make for each one of her children before she left this world. And, she shares the story of Iris, a woman being cared for with terminal cancer who desperately wanted to watch her son graduate from high school. Jeannine shares, “Every time she would try to get up, her pain would get so excruciating that she couldn’t make it through.” Jeannine offered to personally take Iris to the ceremony and administer whatever pain medications she needed just so she could watch her son receive his hard-earned diploma. Not only was Iris able, she had the strength to make an appearance at her son’s graduation party after the event. “Of course, she lasted only a couple of minutes and we had to take her back to the hospital. But to let her do that? Oh my goodness.”
When Jeannine stops to think about the moments she’s shared at the end of a person’s life, she can’t help but get emotional. “It is so amazing that we as nurses get to enter into people’s sacred spaces, to be able to help them in this way. When we look at people at the end of life, Kubler-Ross calls it the final stage of growth. There is some incredible growth that happens at the end of life.”
There have been times when stories of her impact on families have been revealed in unexpected ways.
“One of the greatest stories is from a time I was lecturing at Montana State University College of Nursing. I give a couple of talks up there every year to the new nurses. Afterward, I got an evaluation that said, ‘You don’t know me but you took care of my mother while she was dying. The nurses that helped me during that process are why I am here today and why I went into nursing.’ It gives me chills. It totally gives me chills,” Jeannine says.
While Jeannine always loved impacting one patient at a time, she admits, “I’m a change the world kind of person.” She wanted to use her passion to impact even more lives. She started to volunteer nationally for clinical practice committees. In layman’s terms, she volunteered to help head up different clinical studies that could help not one patient, but many. “I started facilitating some studies at a distance so that Montana patients could enroll in some nursing research studies. The nursing research I found to be very conducive to that human side and looking at patients’ symptoms,” she says. “It was really of interest to me to try to improve that side of care because medicine is really into diagnosing and treating disease. But we, as nurses, care for the human response to the illness.”
It was one more open door for Jeannine to have her hand in change.
Over the course of her 35 year nursing career, Jeannine has headlined national conferences. She’s been mentioned in prominent mainstream magazines like Forbes. She’s been a guest on CNN talking about pain management and palliative care. Her work has been cited in various journals in excess of 500 times. She’s been a speaker at more than 250 events worldwide. The research studies she’s been a key part of have earned more than $1.1 million in grants and financial support. She had a hand editing the book Standards of Practice for Oncology Nursing, which details the standards of care that oncology nurses use in hospitals from coast to coast. Last year, Jeannine Brant was inducted into the American Academy of Nursing, which is basically the nursing hall of fame. Out of more than three million nurses in the United States, only two thousand nurses have made it into this prestigious academy. That’s just a snapshot of her career. If you want the rest of her accomplishments, you’ll find them in her Curriculum Vitae, which is 23 pages long.

Chris Manning is a registered nurse and Outpatient Care Manager with the Billings Clinic. She gave Jeannine her first break in 1984 and hired her as a staff nurse in the oncology unit at what was then Deaconess Medical Center. Chris calls that hire one of her “claims to fame.” She says, “It was easy to see that she had that fresh enthusiasm for nursing and she grew to love the oncology patients.” Even then, she says she knew Jeannine Brant would go places. “I always knew she was destined for success and I have been greatly impressed by how she has done it. She’s a colleague among nursing greats around the country and the world and yet she is ‘Jeannine’ to us – humble and gracious.”
While Jeannine is indeed proud of how she has impacted the field, helping to set up chemotherapy clinics in rural areas all over Montana and profoundly touching lives on eight of Montana’s Indian reservations educating more than 20,000 women and drastically increasing the rates of mammography, her focus now is on the world’s cancer care. It’s through the Middle Eastern Cancer Consortium (MECC) that Jeannine Brant has a direct impact on 19 different countries and how they care for their cancer patients.
“We are not bound by our state lines anymore,” she says excitedly as she talks about her role with MECC. As the Middle Eastern liaison for the Oncology Nursing Society, any education through the Oncology Nursing Society that happens in the Middle East is set up personally by Jeannine. “A lot of love and passion goes into everything I do on behalf of those patients. That gives me such an amazing foundation to go and do what I am doing right now.”

When educational opportunities arise, Jeannine will leave her post as nurse scientist at the Billings Clinic with a team of nurses to put on conferences for her peers in the Middle East. In mid-October, she’s headed to Oman with five other nurses to head up a four-day palliative care course. After Oman, she’ll head to Dubai for yet another conference. Fellow Nurse and longtime friend, Regina Fink, will be with Jeannine to share in the lessons. She’s made the trek with Jeannine to Oman and Turkey in the past. “Jeannine really has a vision for where she wants to see palliative care going in the Middle East. I think of her energy, her commitment, and her dedication. She never seems to lose it. She’s very humble about what she does,” Regina says. “I think that is what makes her remarkable.”
When Jeannine steps through the doors of any conference in the Middle East, all stereotypes are thrown aside. All political beliefs are left at the door. “It's not about politics, it's about relationships. It's putting a face on a country, building relationships and learning about oncology and palliative care at the same time.” It’s a job that she says can be completely grueling. “You’ve never worked so hard in all your life when you go there. We work from morning until night revising the agenda and making sure that we are meeting their needs,” she says. “We are trying to give them the tools that they need so that when they go back to their settings they can make a valuable contribution that's evidence-based.”
Despite the fact that the coalition is made up of 19 mostly Muslim countries, it’s headed up by a Jewish professor, a physician who used to work at the National Institutes of Health. While many wars in the area stem from bitter religious differences, in this group, Dr. Michael Silbermann is more than respected. This man has become like an adored father figure to Jeannine. She still shakes her head in disbelief when she thinks about her role. “I can’t believe I’m in Billings, Montana and I’m doing this stuff. If I sit and think about this too long? It’s mind blowing.”
You’d think that working on worldwide solutions in cancer care would take up all of Jeannine Brant’s time. Not true. She still works three days a week mentoring nurses at the Billings Clinic. She still has a hand in a few national clinical practice committees and on top of that, oversees more than a half dozen clinical studies at the Billings Clinic.
She loves those opportunities when she can touch a new nurse and empower her to push her boundaries to make a difference.
“I had a nurse crying on the unit one day. She was a new oncology nurse and she said to me, ‘Gosh, I am so sorry I am just not handling this well.’ I told her, ‘Don't feel bad about crying for a patient. I am going to worry about you when you stop crying.’” Jeannine goes on to say, “We're dealing with people's lives, we are dealing with their families, we are dealing with them at their most vulnerable moments. So this is a privilege that we've been given as nurses and health care professionals to care for people. We are going to hurt. We are going to care.
That feeling has been passed down to one of Jeannine’s three children. Her 21-year-old daughter Annette is studying to be a nurse. “It’s exciting knowing that my daughter has chosen this path. I am so proud of her,” Jeannine says as she beams. She’s proud though of all her children. Her son, Zach, is a senior this year at Senior High. Her 23-year-old daughter Danielle, is a music major living in Oregon. And, then there’s her husband, a man she calls a “true gem.” She adds, “I wouldn’t be doing all if this if it weren’t for my husband, Rich, supporting me along the way.”
As Jeannine reflects, she knows her career is a far cry from how she envisioned it. She laughs as she says, “I thought I was going to be an ICU nurse. I wanted to be a flight nurse so that I could go rescue people.” Little did she know that her work would rescue so many more lives.
“I am really so humbled by that,” she admits. “I do what I do because I love to do it. I have a lot of thankfulness to the Lord because He gives me the energy. I feel like my cup is pretty full and I try to keep it full so that I can spill out into other people.”
Even she admits she’s not even close to hanging up her white lab coat or ditching her presentation notes.
“I have a passion to inspire people to go out and change the world,” she says with emotion. “That's what I get to do now. I get to be the mentor. I am 53 years old. I still have so much life left!”
LIFE’S LITTLE LESSONS
What Jeannine Brant has learned from her patients
Don’t borrow trouble from tomorrow
Let’s talk about death and dying so we’re not afraid
Live each day to the fullest
Don’t delay. Do things now!
Have a sense of humor