New Weapons in the Fight against Depression
The Struggle to Survive
Dark, overwhelming and heavy doesn’t even begin to describe the depths of despair that seemed to shackle 45-year-old Gretchen Ulrickson for stretches at a time. She would spend days in bed, unable to crawl out to face the world. Depression would settle in and its choke hold on her mood brought suicidal attempts not once, not twice but three times over the past decade.
“I was so adverse to medication. I wasn’t seeing a doctor. I wasn’t being proactive. My only solution was to kill myself,” Gretchen admits. “That’s the only solution I could see.” Even though her father suffered from severe depression to the point of hospitalization, Gretchen never thought she’d follow in his footsteps.
The suicidal thoughts typically were triggered by a traumatic event in her life. The first time, stress on the job pushed her over the edge. Gretchen planned to use her service revolver given to her as a Plentywood police officer to take her life. When thoughts of suicide crept up again, it was after a failed pregnancy. She planned a trip for her husband and mixed up a cocktail of alcohol and opiates. The third stretch came after her husband, her best friend, lost the fight against a brain tumor. Gretchen tried to numb the incredible pain by attempting to slit her wrists. While she doesn’t remember sending the message, she says, “I texted my friend one word and it was ‘Help.’”
For a little more than 30% of those who suffer from moderate to severe depression, help is elusive. Medicines fail. Therapies fail and nothing seems to want to touch the darkness trapped inside.
“I felt like I was hitting a wall with so many people. We had tried so many different things,” Dr. Erin Amato says with passion. Dr. Amato is an adult and child psychiatrist with Montana Psychiatry. After losing her first patient to suicide two years ago, she knew she had to be on the frontline in finding alternative therapies, especially for those who never seemed to find relief.

After Robin William’s suicide captured headlines in 2014, Dr. Amato remembers listening to a news piece on one new off label intervention that has since altered the course of her practice. The drug is Ketamine, an infusion that is often used to start and maintain anesthesia. It’s now showing rapid relief for drug resistant depression.
Major depression affects 6.7% of the population or just shy of 15 million
American adults in any given year
Gretchen Ulrickson is one of Dr. Amato’s success stories.
“When we first met, her depression was so severe, she was on the brink of needing an in-patient hospitalization,” Dr. Amato explains. “She was having severe suicidal thoughts. Her depression was very severe.”
“I was so low, I didn’t know how long I could wait,” Gretchen says. Dr. Amato ultimately wanted to put Gretchen on what is called TMS or Transcranial Magnetic Stimulation, but she needed something to help in the short term. Dr. Amato says, “We knew it would take some time to try to wade through the process dealing with her insurance company but in the meantime, she needed some immediate relief.” Dr. Amato turned to Ketamine and set Gretchen up for six infusions over a two-week course of treatment.
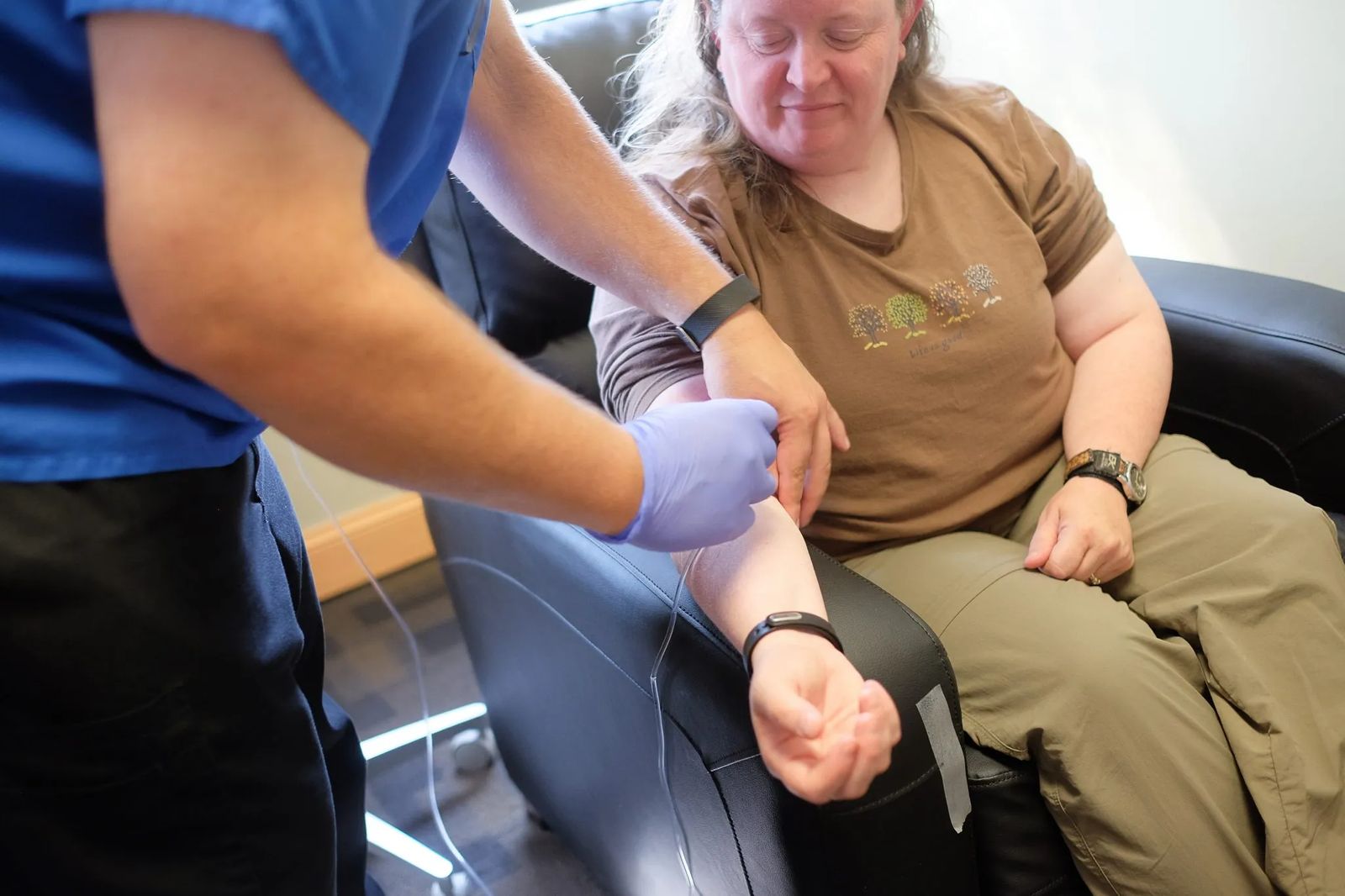
“Something after that third treatment just lifted in me. It is so hard to describe,” Gretchen explains. “It was this sense of ‘Oh my God, this is who I am! This is who I really am. I am me again.’ I was able to maintain control of myself again.”
Ketamine is an infusion that takes roughly 40 minutes to deliver. Seventy percent of the patients who undergo this therapy see those self-harming thoughts start to disappear. Dr. Amato says the drug works on the neurotransmitter level. “The research suggests that Ketamine is working to repair damage to the brain that may have occurred as a result of chronic stress, a traumatic event or the long term effects of depression.” She explains what it’s like to witness this kind of transformation. “For someone to have suicidal thoughts and impulses and then go in to have a ketamine infusion, come out of it several hours later and feel a significant decrease in their suicidal thoughts, it’s a game changer for us.” She is quick to add, “In terms of medication therapies, it’s been a long time since we’ve had something really novel, something really new. I think that’s why Ketamine is causing quite a stir in the psychiatric world.”
Unfortunately, because treating depression with Ketamine is an “off label” use of the drug, insurance companies won’t cover the therapy. A series of six infusions can cost anywhere from $3,000 to $6,000. Dr. Amato would love the FDA to embrace this as a major tool to target drug resistant depression. She says, “What is the cost to someone with an inpatient hospitalization? What is the cost in terms of days of work missed because you are so depressed that you can’t get out of bed or the price tag on the lost life, the lost quality of relationships in your interactions with family and friends?”
For Gretchen, the Ketamine treatments bought her time so she could eventually move into TMS therapy.
“It has been so gratifying and humbling to see the change in how she looked when she first came to us and how she is doing now. It just motivates me even further to keep pressing on with trying to find new and innovative treatments that are going to help people,” Dr. Amato says with a smile.
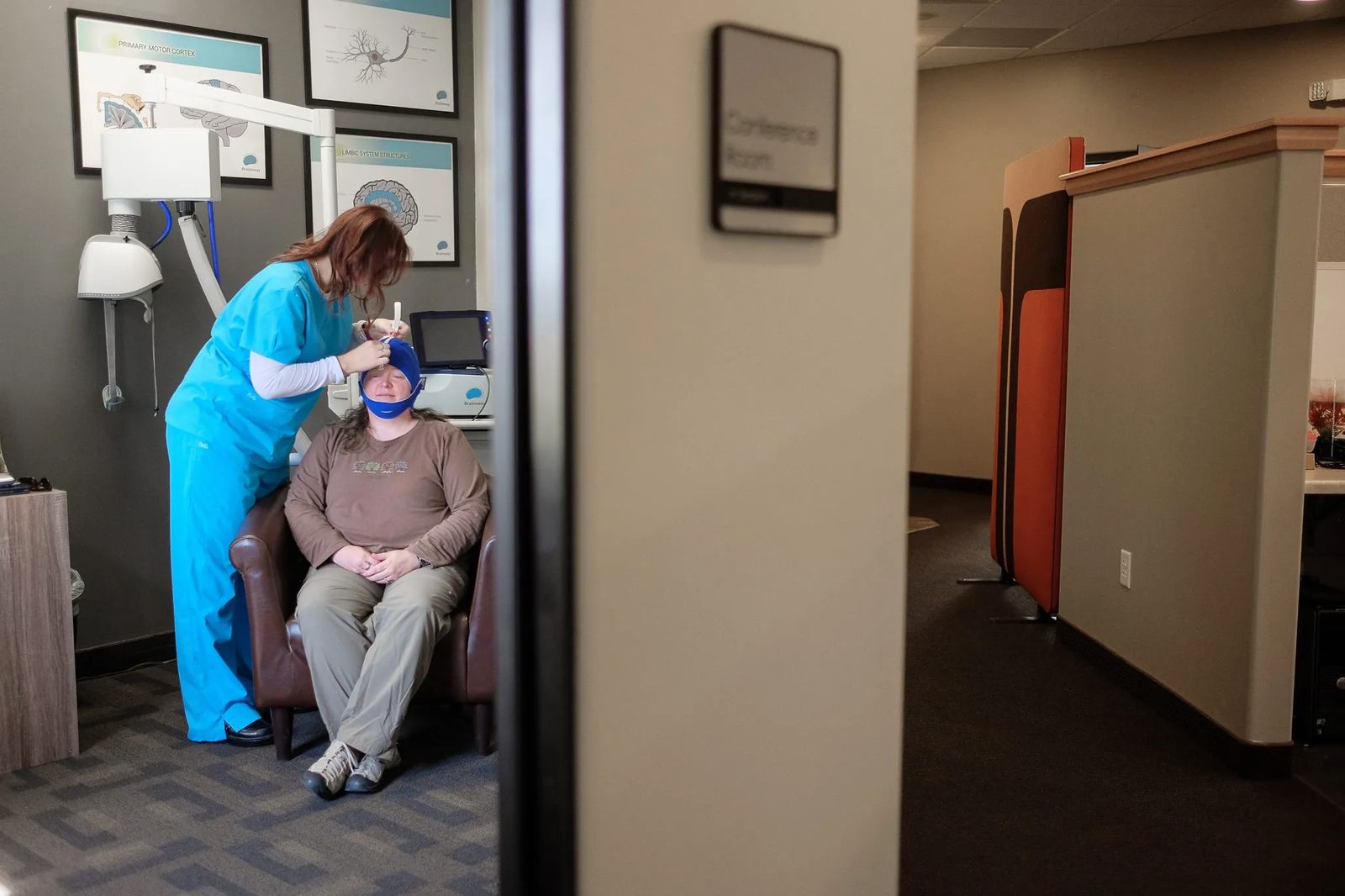
TMS, the second part of Gretchen’s treatment, works by sparking a reaction in the brain without medication. Dr. Amato says, “The brain is both a chemical and an electrical organ. And so, TMS works by delivering MRI strength magnetic pulses over an area of the brain that tends to be inactive or sluggish in people who have depression. The stimulation helps to generate more activity in that area.” According to one clinical trial, 50% of those treated did something they never thought possible. They achieved full remission from major depression. “I have seen some people do TMS and then, I have not had them return for any further treatment. It is amazing,” Dr. Amato says.
Women experience depression at twice the rate of men – 26% of women
will experience it in their lifetime
With success stories like Gretchen, Dr. Amato is proud to be the first in the region to offer what she calls these innovative therapies. Her patients no longer have to travel to Seattle or Denver to try to break the cycle of darkness that depression delivers.
“Now we can say we have new options, new treatments that are available to you. You see people light up because there is some renewed hope that there may be something else to try. It is very invigorating,” Dr. Amato says.
Gretchen just wrapped up her final TMS treatment. After suffering for ten years with deep depression and suicidal thoughts, her outlook on life now includes something she hasn’t seen in years — hope for the future. She’s started riding her bike again, something she used to love to do, and once again finds joy in her family. With tears welling in her eyes, she says, “I feel like I can do this. I can actually do this. I can live!”
Are Ketamine or TMS Therapies an option?
In order to pursue this kind of therapy, Dr. Erin Amato says patients should have moderate to severe depression and have previously suffered at least two drug failures before she would pursue these therapies.
THE SIGNS OF DEPRESSION
When these symptoms emerge, it’s time to talk to your doctor
- Prolonged sadness, unexplained crying spells
- Changes in appetite and sleep patterns
- Irritability, anger, anxiety
- Feelings of worthlessness
- Social withdrawal and an inability to take pleasure in interests
- Unexplained aches and pains
- Recurring thoughts of suicide